IVF (In Vitro Fertilization)
Assisted reproductive technology (ART) includes in vitro fertilization (IVF), gamete intrafallopian tube transfer (GIFT) and zygote intrafallopian tube transfer (ZIFT). GIFT and ZIFT are now rarely performed due to higher costs and lower success rates than IVF. For IVF, the patient is stimulated with medicine to make several eggs grow within the ovary. The eggs are then collected through the vagina using a sonogram-guided needle under sedation. Sperm is then added to the eggs to allow fertilization to take place. Fertilized eggs are then placed back in the uterus a few days later. IVF is effective for different types of infertility including tubal disease, male factor, ovulation disorders, endometriosis and unexplained infertility.
What effect does female age have on getting pregnant and staying pregnant?
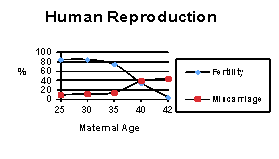 Fertility rates decline with age. Although the average age of menopause is 53, most women are not very fertile after age 40. Miscarriage rates also rise with age. Lastly, pregnant women over 35 years have a higher rate of chromosome abnormalities such as Down Syndrome. Women over 40 years old are encouraged to have a clomiphene citrate challenge test or other test of ovarian reserve function to determine egg quality before doing IVF.
Fertility rates decline with age. Although the average age of menopause is 53, most women are not very fertile after age 40. Miscarriage rates also rise with age. Lastly, pregnant women over 35 years have a higher rate of chromosome abnormalities such as Down Syndrome. Women over 40 years old are encouraged to have a clomiphene citrate challenge test or other test of ovarian reserve function to determine egg quality before doing IVF.
Male Factor Procedures – If the husband has a normal semen analysis, then sperm are simply added to the eggs and natural fertilization occurs. However, if the semen analysis is abnormal then intracytoplasmic sperm injection (ICSI) is indicated. ICSI is a technique where a single sperm is injected directly into the cytoplasm (center) of the egg.
 Risks associated with offspring born from ICSI procedures are still under investigation. While currently available data suggest that the risk of birth defects or major congenital defects in children born from ICSI is approximately that of the general population (approximately 3-4%), it is possible that such defects could occur as a result of the procedure. A higher incidence of abnormalities with the Y chromosome in male offspring (2-3% vs. background rate of 0.1-0.5%) from ICSI in men with very low sperm counts has been noted. While the implications of such findings remain unclear, it is possible that male offspring may be at higher risk of fertility problems if such abnormalities occur. The Y chromosome defects are not from the ICSI procedure itself but from the genetic information being passed on that has resulted in a low sperm count to begin with. There also is a slight increased risk of sex chromosomal abnormalities from the ICSI procedure (0.8% vs. background rate of 0.23%) such as Klinefelter’s Syndrome and Turner’s Syndrome. Because ICSI is still a relatively new procedure, there may be additional risks that cannot be foreseen at present.
Risks associated with offspring born from ICSI procedures are still under investigation. While currently available data suggest that the risk of birth defects or major congenital defects in children born from ICSI is approximately that of the general population (approximately 3-4%), it is possible that such defects could occur as a result of the procedure. A higher incidence of abnormalities with the Y chromosome in male offspring (2-3% vs. background rate of 0.1-0.5%) from ICSI in men with very low sperm counts has been noted. While the implications of such findings remain unclear, it is possible that male offspring may be at higher risk of fertility problems if such abnormalities occur. The Y chromosome defects are not from the ICSI procedure itself but from the genetic information being passed on that has resulted in a low sperm count to begin with. There also is a slight increased risk of sex chromosomal abnormalities from the ICSI procedure (0.8% vs. background rate of 0.23%) such as Klinefelter’s Syndrome and Turner’s Syndrome. Because ICSI is still a relatively new procedure, there may be additional risks that cannot be foreseen at present.
On which day should the embryos be placed back into the uterus?
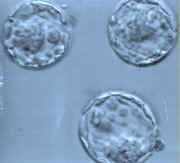
Initially, fertilized eggs were transferred back to the uterus after 1 day. Research then showed that transfer on day 2-3 was better. A few years ago, some studies showed that transfer back on day 5-6 was better still. On day 5-6, developing embryos are called blastocysts. However, more recent studies have shown that while blastocyst transfer is better in certain situations, day 2-3 transfer is still better for some patients. The optimal day for your embryo transfer will be decided upon by the embryologist and your physician as the embryos develop. Extra viable embryos may be successfully frozen at different stages for later use.
Ovarian hyperstimulation syndrome occurs in about 5% of patients. Approximately 5% of patients undergoing ART will develop ovarian hyperstimulation syndrome. This occurs when the ovaries are extremely sensitive to the fertility medication and become quite enlarged and swollen. If this occurs, most patients are successfully treated at home on bed rest, but rare patients have to be hospitalized. One value of the blood estrogen testing and vaginal sonograms is that individuals at high risk for developing this hyperstimulation syndrome can be identified. Rarely, enlarged ovaries can become twisted (ovarian torsion) which may require surgical removal.
ART babies may have more birth defects . The background risk for birth defects is 3-4%. IVF may increase the risk of birth defects as high as 6-8%. IVF pregnancies are high risk. There is an increased chance for pre-term delivery, low birth weight, birth defects, chromosomal abnormalities, brain damage and death. There may be an increased risk of genetic diseases. Increased maternal complications can also occur such as preeclampsia, placental abruption and need for C-section. . Any patient over age 35 is at an increased risk for chromosomal abnormalities such as Down Syndrome and should consider a genetic amniocentesis if pregnancy occurs.
ART pregnancies may end in either a miscarriage or an ectopic pregnancy.
The chance for miscarriage is slightly reduced with IVF since supplemental progesterone is used and certain non-viable embryo abnormalities are eliminated and not transferred such as triploidy. Overall, miscarriage rates increase with maternal age. The chance for a tubal or ectopic pregnancy is about 1-2%. Embryos circulate within the uterus for a few days prior to implanting and rarely can become lodged in a fallopian tube. Tubal pregnancies require either surgical or medical intervention.
The medications used in ART possibly are associated with ovarian cancer . An epidemiological study in the early 1990’s suggested that Pergonal use might increase the chances for developing ovarian cancer later in life. However, many more recent studies do not agree. Patients who have infertility already have a higher chance of getting ovarian cancer on the basis of the infertility alone and it is difficult to separate out the various risk factors. Clearly, more study is needed on this matter before definitive conclusions can be made about Pergonal either way. Gonal-F, Follistim, Bravelle, Repronex and Menopur are very similar medications to Pergonal and these concerns may also apply to them.
